Boxed Warning
Hyperkalemia:
Abnormal elevation of serum potassium levels (5.5 mEq/L or more) can occur with hydrochlorothiazide/triamterene. Hyperkalemia is more likely to occur in patients with renal impairment and diabetes (even without evidence of renal impairment), or elderly or severely ill patients. Because uncorrected hyperkalemia may be fatal, serum potassium levels must be monitored at frequent intervals, especially in patients first receiving hydrochlorothiazide/triamterene, when dosages are changed, or with any illness that may influence renal function.
Dosage Forms
Excipient information presented when available (limited, particularly for generics); consult specific product labeling.
Capsule, Oral:
Dyazide: Hydrochlorothiazide 25 mg and triamterene 37.5 mg
Generic: Hydrochlorothiazide 25 mg and triamterene 37.5 mg
Tablet, Oral:
Maxzide: Hydrochlorothiazide 50 mg and triamterene 75 mg [scored]
Maxzide-25: Hydrochlorothiazide 25 mg and triamterene 37.5 mg [scored]
Generic: Hydrochlorothiazide 25 mg and triamterene 37.5 mg; Hydrochlorothiazide 50 mg and triamterene 75 mg
Pharmacology
Mechanism of Action
Hydrochlorothiazide: Inhibits sodium reabsorption in the distal tubules causing increased excretion of sodium and water as well as potassium and hydrogen ions.
Triamterene: Blocks epithelial sodium channels in the late distal convoluted tubule (DCT) and collecting duct which inhibits sodium reabsorption from the lumen. This effectively reduces intracellular sodium, decreasing the function of Na+/K+ ATPase, leading to potassium retention and decreased calcium, magnesium, and hydrogen excretion. As sodium uptake capacity in the DCT/collecting duct is limited, the natriuretic, diuretic, and antihypertensive effects are generally considered weak.
Use: Labeled Indications
Hypertension, edema: Treatment of hypertension or edema (not recommended for initial treatment) when hypokalemia has developed on hydrochlorothiazide alone or when the development of hypokalemia must be avoided.
Contraindications
Hypersensitivity to hydrochlorothiazide, triamterene, sulfonamide-derived drugs, or any component of the formulation; anuria; acute and chronic renal insufficiency or significant renal impairment; patients receiving other potassium-sparing diuretics, potassium-containing salt substitutes, or potassium supplements (except in severe cases of hypokalemia); preexisting hyperkalemia
Note: Although the FDA approved product labeling states this medication is contraindicated with other sulfonamide-containing drug classes, the scientific basis of this statement has been challenged. See “Warnings/Precautions” for more detail.
Canadian labeling: Additional contraindications (not in US labeling): Severe or progressive hepatic dysfunction
Dosage and Administration
Dosing: Adult
Hypertension, edema: Oral:
Hydrochlorothiazide 25 mg/triamterene 37.5 mg: 1 to 2 tablets/capsules once daily
Hydrochlorothiazide 25 mg/triamterene 50 mg: 1 to 2 capsules once daily
Hydrochlorothiazide 50 mg/triamterene 75 mg: 1 tablet daily
Dosing: Geriatric
Refer to adult dosing.
Administration
Oral: Administer without regard to meals.
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F). Protect from light.
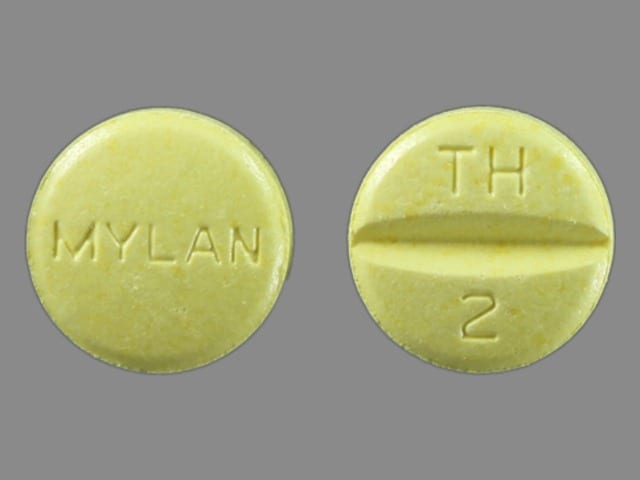
Hydrochlorothiazide and Triamterene Images
Drug Interactions
Ajmaline: Sulfonamides may enhance the adverse/toxic effect of Ajmaline. Specifically, the risk for cholestasis may be increased. Monitor therapy
Alcohol (Ethyl): May enhance the orthostatic hypotensive effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Alfuzosin: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Allopurinol: Thiazide and Thiazide-Like Diuretics may enhance the potential for allergic or hypersensitivity reactions to Allopurinol. Thiazide and Thiazide-Like Diuretics may increase the serum concentration of Allopurinol. Specifically, Thiazide Diuretics may increase the concentration of Oxypurinol, an active metabolite of Allopurinol. Monitor therapy
Amifostine: Blood Pressure Lowering Agents may enhance the hypotensive effect of Amifostine. Management: When amifostine is used at chemotherapy doses, blood pressure lowering medications should be withheld for 24 hours prior to amifostine administration. If blood pressure lowering therapy cannot be withheld, amifostine should not be administered. Consider therapy modification
Aminolevulinic Acid (Systemic): Photosensitizing Agents may enhance the photosensitizing effect of Aminolevulinic Acid (Systemic). Avoid combination
Aminolevulinic Acid (Topical): Photosensitizing Agents may enhance the photosensitizing effect of Aminolevulinic Acid (Topical). Monitor therapy
Ammonium Chloride: Potassium-Sparing Diuretics may enhance the adverse/toxic effect of Ammonium Chloride. Specifically the risk of systemic acidosis. Consider therapy modification
Amphetamines: May diminish the antihypertensive effect of Antihypertensive Agents. Monitor therapy
Angiotensin II Receptor Blockers: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Monitor therapy
Angiotensin-Converting Enzyme Inhibitors: Potassium-Sparing Diuretics may enhance the hyperkalemic effect of Angiotensin-Converting Enzyme Inhibitors. Monitor therapy
Angiotensin-Converting Enzyme Inhibitors: Thiazide and Thiazide-Like Diuretics may enhance the hypotensive effect of Angiotensin-Converting Enzyme Inhibitors. Thiazide and Thiazide-Like Diuretics may enhance the nephrotoxic effect of Angiotensin-Converting Enzyme Inhibitors. Monitor therapy
Anticholinergic Agents: May increase the serum concentration of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Antidiabetic Agents: Thiazide and Thiazide-Like Diuretics may diminish the therapeutic effect of Antidiabetic Agents. Monitor therapy
Antidiabetic Agents: Hyperglycemia-Associated Agents may diminish the therapeutic effect of Antidiabetic Agents. Monitor therapy
Antipsychotic Agents (Second Generation [Atypical]): Blood Pressure Lowering Agents may enhance the hypotensive effect of Antipsychotic Agents (Second Generation [Atypical]). Monitor therapy
Barbiturates: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Benazepril: HydroCHLOROthiazide may enhance the hypotensive effect of Benazepril. HydroCHLOROthiazide may enhance the nephrotoxic effect of Benazepril. Benazepril may decrease the serum concentration of HydroCHLOROthiazide. Monitor therapy
Benperidol: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Beta2-Agonists: May enhance the hypokalemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Bile Acid Sequestrants: May decrease the absorption of Thiazide and Thiazide-Like Diuretics. The diuretic response is likewise decreased. Consider therapy modification
Brigatinib: May diminish the antihypertensive effect of Antihypertensive Agents. Brigatinib may enhance the bradycardic effect of Antihypertensive Agents. Monitor therapy
Brimonidine (Topical): May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Bromperidol: Blood Pressure Lowering Agents may enhance the hypotensive effect of Bromperidol. Bromperidol may diminish the hypotensive effect of Blood Pressure Lowering Agents. Avoid combination
Calcium Salts: Thiazide and Thiazide-Like Diuretics may decrease the excretion of Calcium Salts. Continued concomitant use can also result in metabolic alkalosis. Monitor therapy
CarBAMazepine: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of CarBAMazepine. Specifically, there may be an increased risk for hyponatremia. Monitor therapy
Cardiac Glycosides: Potassium-Sparing Diuretics may diminish the therapeutic effect of Cardiac Glycosides. In particular, the inotropic effects of digoxin appear to be diminished. Potassium-Sparing Diuretics may increase the serum concentration of Cardiac Glycosides. This particular effect may be unique to Spironolactone. Monitor therapy
Cardiac Glycosides: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of Cardiac Glycosides. Specifically, cardiac glycoside toxicity may be enhanced by the hypokalemic and hypomagnesemic effect of thiazide diuretics. Monitor therapy
Corticosteroids (Orally Inhaled): May enhance the hypokalemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Corticosteroids (Systemic): May enhance the hypokalemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Cyclophosphamide: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of Cyclophosphamide. Specifically, granulocytopenia may be enhanced. Monitor therapy
CycloSPORINE (Systemic): Potassium-Sparing Diuretics may enhance the hyperkalemic effect of CycloSPORINE (Systemic). Avoid combination
Dexketoprofen: May enhance the adverse/toxic effect of Sulfonamides. Monitor therapy
Dexmethylphenidate: May diminish the therapeutic effect of Antihypertensive Agents. Monitor therapy
Diacerein: May enhance the therapeutic effect of Diuretics. Specifically, the risk for dehydration or hypokalemia may be increased. Monitor therapy
Diazoxide: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of Diazoxide. Monitor therapy
Diazoxide: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Dichlorphenamide: Thiazide and Thiazide-Like Diuretics may enhance the hypokalemic effect of Dichlorphenamide. Monitor therapy
Dofetilide: HydroCHLOROthiazide may enhance the QTc-prolonging effect of Dofetilide. HydroCHLOROthiazide may increase the serum concentration of Dofetilide. Avoid combination
Drospirenone: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Monitor therapy
DULoxetine: Blood Pressure Lowering Agents may enhance the hypotensive effect of DULoxetine. Monitor therapy
Eplerenone: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Management: This combination is contraindicated in patients receiving eplerenone for treatment of hypertension. Consider therapy modification
Fexinidazole [INT]: Thiazide and Thiazide-Like Diuretics may enhance the arrhythmogenic effect of Fexinidazole [INT]. Avoid combination
Heparin: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Management: Monitor serum potassium concentrations closely. The spironolactone Canadian product monograph lists its combination with heparin or low molecular weight heparins as contraindicated. Monitor therapy
Heparins (Low Molecular Weight): May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Management: Monitor serum potassium concentrations closely. The spironolactone Canadian product monograph lists its combination with heparin or low molecular weight heparins as contraindicated. Monitor therapy
Herbs (Hypertensive Properties): May diminish the antihypertensive effect of Antihypertensive Agents. Monitor therapy
Herbs (Hypotensive Properties): May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Hypotension-Associated Agents: Blood Pressure Lowering Agents may enhance the hypotensive effect of Hypotension-Associated Agents. Monitor therapy
Indomethacin: May enhance the nephrotoxic effect of Triamterene. Management: Consider alternatives to concomitant treatment with triamterene and indomethacin. If the combination cannot be avoided, monitor for development of renal failure. Consider therapy modification
Ipragliflozin: May enhance the adverse/toxic effect of Thiazide and Thiazide-Like Diuretics. Specifically, the risk for intravascular volume depletion may be increased. Monitor therapy
Ivabradine: Thiazide and Thiazide-Like Diuretics may enhance the arrhythmogenic effect of Ivabradine. Monitor therapy
Levodopa-Containing Products: Blood Pressure Lowering Agents may enhance the hypotensive effect of Levodopa-Containing Products. Monitor therapy
Levosulpiride: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of Levosulpiride. Avoid combination
Licorice: May enhance the hypokalemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Lithium: Thiazide and Thiazide-Like Diuretics may decrease the excretion of Lithium. Consider therapy modification
Lormetazepam: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Mecamylamine: Sulfonamides may enhance the adverse/toxic effect of Mecamylamine. Avoid combination
Methenamine: Thiazide and Thiazide-Like Diuretics may diminish the therapeutic effect of Methenamine. Monitor therapy
Methylphenidate: May diminish the antihypertensive effect of Antihypertensive Agents. Monitor therapy
Molsidomine: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Multivitamins/Fluoride (with ADE): May enhance the hypercalcemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Multivitamins/Minerals (with ADEK, Folate, Iron): Thiazide and Thiazide-Like Diuretics may enhance the hypercalcemic effect of Multivitamins/Minerals (with ADEK, Folate, Iron). Monitor therapy
Multivitamins/Minerals (with AE, No Iron): Thiazide and Thiazide-Like Diuretics may increase the serum concentration of Multivitamins/Minerals (with AE, No Iron). Specifically, thiazide diuretics may decrease the excretion of calcium, and continued concomitant use can also result in metabolic alkalosis. Monitor therapy
Naftopidil: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Neuromuscular-Blocking Agents (Nondepolarizing): Thiazide and Thiazide-Like Diuretics may enhance the neuromuscular-blocking effect of Neuromuscular-Blocking Agents (Nondepolarizing). Monitor therapy
Nicergoline: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Nicorandil: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Monitor therapy
Nicorandil: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Nitroprusside: Blood Pressure Lowering Agents may enhance the hypotensive effect of Nitroprusside. Monitor therapy
Nonsteroidal Anti-Inflammatory Agents: Thiazide and Thiazide-Like Diuretics may enhance the nephrotoxic effect of Nonsteroidal Anti-Inflammatory Agents. Nonsteroidal Anti-Inflammatory Agents may diminish the therapeutic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Nonsteroidal Anti-Inflammatory Agents: May diminish the antihypertensive effect of Potassium-Sparing Diuretics. Nonsteroidal Anti-Inflammatory Agents may enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Monitor therapy
Obinutuzumab: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Management: Consider temporarily withholding blood pressure lowering medications beginning 12 hours prior to obinutuzumab infusion and continuing until 1 hour after the end of the infusion. Consider therapy modification
Opioid Agonists: May enhance the adverse/toxic effect of Diuretics. Opioid Agonists may diminish the therapeutic effect of Diuretics. Monitor therapy
OXcarbazepine: Thiazide and Thiazide-Like Diuretics may enhance the adverse/toxic effect of OXcarbazepine. Specifically, there may be an increased risk for hyponatremia. Monitor therapy
Pentoxifylline: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Pholcodine: Blood Pressure Lowering Agents may enhance the hypotensive effect of Pholcodine. Monitor therapy
Phosphodiesterase 5 Inhibitors: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Porfimer: Photosensitizing Agents may enhance the photosensitizing effect of Porfimer. Monitor therapy
Potassium Salts: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Consider therapy modification
Promazine: Thiazide and Thiazide-Like Diuretics may enhance the QTc-prolonging effect of Promazine. Avoid combination
Prostacyclin Analogues: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
Quinagolide: May enhance the hypotensive effect of Blood Pressure Lowering Agents. Monitor therapy
QuiNIDine: Potassium-Sparing Diuretics may diminish the therapeutic effect of QuiNIDine. Monitor therapy
Reboxetine: May enhance the hypokalemic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Selective Serotonin Reuptake Inhibitors: May enhance the hyponatremic effect of Thiazide and Thiazide-Like Diuretics. Monitor therapy
Sodium Phosphates: Diuretics may enhance the nephrotoxic effect of Sodium Phosphates. Specifically, the risk of acute phosphate nephropathy may be enhanced. Management: Consider avoiding this combination by temporarily suspending treatment with diuretics, or seeking alternatives to oral sodium phosphate bowel preparation. If the combination cannot be avoided, hydrate adequately and monitor fluid and renal status. Consider therapy modification
Spironolactone: Triamterene may enhance the hyperkalemic effect of Spironolactone. Avoid combination
Tacrolimus (Systemic): Potassium-Sparing Diuretics may enhance the hyperkalemic effect of Tacrolimus (Systemic). Monitor therapy
Tolvaptan: May enhance the hyperkalemic effect of Potassium-Sparing Diuretics. Monitor therapy
Topiramate: Thiazide and Thiazide-Like Diuretics may enhance the hypokalemic effect of Topiramate. Thiazide and Thiazide-Like Diuretics may increase the serum concentration of Topiramate. Management: Monitor for increased topiramate levels/adverse effects (e.g., hypokalemia) with initiation/dose increase of a thiazide diuretic. Closely monitor serum potassium concentrations with concomitant therapy. Topiramate dose reductions may be necessary. Consider therapy modification
Toremifene: Thiazide and Thiazide-Like Diuretics may enhance the hypercalcemic effect of Toremifene. Monitor therapy
Valsartan: HydroCHLOROthiazide may enhance the hypotensive effect of Valsartan. Valsartan may increase the serum concentration of HydroCHLOROthiazide. Monitor therapy
Verteporfin: Photosensitizing Agents may enhance the photosensitizing effect of Verteporfin. Monitor therapy
Vitamin D Analogs: Thiazide and Thiazide-Like Diuretics may enhance the hypercalcemic effect of Vitamin D Analogs. Monitor therapy
Yohimbine: May diminish the antihypertensive effect of Antihypertensive Agents. Monitor therapy
Test Interactions
See individual agents.
Adverse Reactions
Also see individual agents. Frequency not defined.
Cardiovascular: Angina pectoris, cardiac arrhythmia, necrotizing angiitis, orthostatic hypotension, tachycardia
Central nervous system: Anxiety, depression, dizziness, fatigue, glossopyrosis, headache, insomnia, paresthesia, restlessness, vertigo
Dermatologic: Skin photosensitivity, skin rash, urticaria
Endocrine & metabolic: Acidosis, diabetes mellitus, glycosuria, hypercalcemia, hyperglycemia, hyperkalemia, hyperuricemia, hypochloremia, hypokalemia, hypomagnesemia, hyponatremia
Gastrointestinal: Abdominal pain, anorexia, constipation, diarrhea, dysgeusia, gastric distress, nausea, pancreatitis, sialadenitis, stomach cramps, tongue discoloration (bright orange), vomiting, xerostomia
Genitourinary: Impotence, urine discoloration, urine sedimentation abnormality
Hematologic & oncologic: Agranulocytosis, aplastic anemia, hemolytic anemia, leukopenia, megaloblastic anemia, purpura, thrombocytopenia
Hepatic: Abnormal liver function tests, jaundice
Hypersensitivity: Anaphylaxis
Neuromuscular & skeletal: Exacerbation of systemic lupus erythematosus, lupus-like syndrome (subacute, cutaneous), muscle cramps, weakness
Ophthalmic: Transient blurred vision, xanthopsia
Renal: Acute renal failure, increased blood urea nitrogen, increased serum creatinine, interstitial nephritis, nephrolithiasis
Respiratory: Dyspnea, hypersensitivity pneumonitis, pulmonary edema, respiratory distress
Miscellaneous: Fever
<1%, postmarketing, and/or case reports: Malignant neoplasm of lip (Friedman 2012)
Warnings/Precautions
Concerns related to adverse effects:
- Electrolyte disturbances: Hypokalemia, hypochloremic alkalosis, and hyponatremia may occur with hydrochlorothiazide.
- Gout: In certain patients with a history of gout, a familial predisposition to gout, or chronic renal failure, gout can be precipitated by hydrochlorothiazide. This risk may be increased with doses ≥25 mg (Gurwitz 1997).
- Hyperkalemia: [US Boxed Warning]: Hyperkalemia can occur with triamterene; patients at risk include those with renal impairment, diabetes (even without evidence of renal impairment), the elderly, and the severely ill. Serum potassium levels must be monitored at frequent intervals especially in patients first receiving hydrochlorothiazide/triamterene, when dosages are changed, or with any illness that may influence renal function. Avoid potassium supplements (except in severe cases of hypokalemia), potassium-containing salt substitutes, a diet rich in potassium, or other drugs that can cause hyperkalemia. Discontinue immediately if hyperkalemia develops. Patients who are severely ill may develop respiratory or metabolic acidosis which may be associated with rapid elevations in serum potassium concentrations; avoid use in these patients.
- Hypersensitivity reactions: Hypersensitivity reactions may occur with hydrochlorothiazide. Risk is increased in patients with a history of allergy or bronchial asthma.
- Ocular effects: Hydrochlorothiazide may cause acute transient myopia and acute angle-closure glaucoma, typically occurring within hours to weeks following initiation; discontinue therapy immediately in patients with acute decreases in visual acuity or ocular pain. Additional treatments may be needed if uncontrolled intraocular pressure persists. Risk factors may include a history of sulfonamide or penicillin allergy.
- Photosensitivity: Photosensitization may occur.
- Sulfonamide (“sulfa”) allergy: The FDA-approved product labeling for many medications containing a sulfonamide chemical group includes a broad contraindication in patients with a prior allergic reaction to sulfonamides. There is a potential for cross-reactivity between members of a specific class (eg, two antibiotic sulfonamides). However, concerns for cross-reactivity have previously extended to all compounds containing the sulfonamide structure (SO2NH2). An expanded understanding of allergic mechanisms indicates cross-reactivity between antibiotic sulfonamides and nonantibiotic sulfonamides may not occur or at the very least this potential is extremely low (Brackett 2004; Johnson 2005; Slatore 2004; Tornero 2004). In particular, mechanisms of cross-reaction due to antibody production (anaphylaxis) are unlikely to occur with nonantibiotic sulfonamides. T-cell-mediated (type IV) reactions (eg, maculopapular rash) are less well understood and it is not possible to completely exclude this potential based on current insights. In cases where prior reactions were severe (Stevens-Johnson syndrome/TEN), some clinicians choose to avoid exposure to these classes.
Disease-related concerns:
- Bariatric surgery: Dehydration: Avoid diuretics in the immediate postoperative period after bariatric surgery; electrolyte disturbances and dehydration may occur. Diuretics may be resumed, if indicated, once oral fluid intake goals are met (Ziegler 2009).
- Diabetes: Use with caution in patients with prediabetes or diabetes mellitus; may alter glycemic control.
- Hepatic impairment: Use caution in patients with severe hepatic impairment. In progressive or severe liver disease, avoid electrolyte and acid/base imbalances that might lead to hepatic encephalopathy/coma.
- Hypercalcemia: Thiazide diuretics may decrease renal calcium excretion; consider avoiding use in patients with hypercalcemia.
- Hypercholesterolemia: Use with caution in patients with moderate or high cholesterol concentrations; increased cholesterol and triglyceride levels have been reported with thiazides.
- Kidney stones: Use triamterene with caution in patients with kidney stones.
- Parathyroid disease: Thiazide diuretics reduce calcium excretion; pathologic changes in the parathyroid glands with hypercalcemia and hypophosphatemia have been observed with prolonged use. Thiazides should be discontinued prior to tests for parathyroid function.
- Renal impairment: Cumulative effects of hydrochlorothiazide may develop, including azotemia, in patients with impaired renal function. Avoid hydrochlorothiazide in severe renal disease (ineffective). Triamterene may cause hyperkalemia in patients with renal impairment.
- Systemic lupus erythematosus (SLE): Hydrochlorothiazide may cause SLE exacerbation or activation.
Concurrent drug therapy issues:
- Drug-drug interactions: Potentially significant interactions may exist, requiring dose or frequency adjustment, additional monitoring, and/or selection of alternative therapy. Consult drug interactions database for more detailed information.
Monitoring Parameters
Monitor blood pressure, serum electrolytes, BUN, creatinine, liver function tests, signs of hyperkalemia
Pregnancy
Pregnancy Risk Factor
C
Pregnancy Considerations
Animal reproduction studies have not been conducted with this combination product. See individual agents.
Patient Education
What is this drug used for?
- It is used to treat high blood pressure.
- It is used to get rid of extra fluid.
Frequently reported side effects of this drug
- Diarrhea
- Dizziness
- Fatigue
- Lack of appetite
- Increased hunger
- Change in taste
- Abdominal cramps
- Constipation
- Headache
- Vomiting
- Nausea
Other side effects of this drug: Talk with your doctor right away if you have any of these signs of:
- Fluid and electrolyte problems like mood changes, confusion, muscle pain or weakness, abnormal heartbeat, severe dizziness, passing out, fast heartbeat, increased thirst, seizures, loss of strength and energy, lack of appetite, unable to pass urine or change in amount of urine passed, dry mouth, dry eyes, nausea, or vomiting.
- Acidosis like confusion, fast breathing, fast heartbeat, abnormal heartbeat, severe abdominal pain, nausea, vomiting, fatigue, shortness of breath, or loss of strength and energy.
- High blood sugar like confusion, fatigue, increased thirst, increased hunger, passing a lot of urine, flushing, fast breathing, or breath that smells like fruit.
- Kidney problems like unable to pass urine, blood in the urine, change in amount of urine passed, or weight gain.
- Pancreatitis like severe abdominal pain, severe back pain, severe nausea, or vomiting.
- Kidney stone like back pain, abdominal pain, or blood in the urine.
- Lupus like rash on the cheeks or other body parts, sunburn easy, muscle or joint pain, chest pain or shortness of breath, or swelling in the arms or legs.
- Infection
- Yellow skin
- Dark urine
- Burning or numbness feeling
- Slow heartbeat
- Agitation
- Bruising
- Bleeding
- Severe loss of strength and energy
- Shortness of breath
- Chest pain
- Fast heartbeat
- Mood changes
- Sexual dysfunction
- Skin changes
- Vision changes
- Eye pain
- Signs of a significant reaction like wheezing; chest tightness; fever; itching; bad cough; blue skin color; seizures; or swelling of face, lips, tongue, or throat.
Note: This is not a comprehensive list of all side effects. Talk to your doctor if you have questions.
Consumer Information Use and Disclaimer: This information should not be used to decide whether or not to take this medicine or any other medicine. Only the healthcare provider has the knowledge and training to decide which medicines are right for a specific patient. This information does not endorse any medicine as safe, effective, or approved for treating any patient or health condition. This is only a brief summary of general information about this medicine. It does NOT include all information about the possible uses, directions, warnings, precautions, interactions, adverse effects, or risks that may apply to this medicine. This information is not specific medical advice and does not replace information you receive from the healthcare provider. You must talk with the healthcare provider for complete information about the risks and benefits of using this medicine.