Atrial fibrillation (A-fib) is an irregular and often very rapid heart rhythm (arrhythmia) that can lead to blood clots in the heart. A-fib increases the risk of stroke, heart failure and other heart-related complications.
During atrial fibrillation, the heart's upper chambers (the atria) beat chaotically and irregularly — out of sync with the lower chambers (the ventricles) of the heart. For many people, A-fib may have no symptoms. However, A-fib may cause a fast, pounding heartbeat (palpitations), shortness of breath or weakness.
Episodes of atrial fibrillation may come and go, or they may be persistent. Although A-fib itself usually isn't life-threatening, it's a serious medical condition that requires proper treatment to prevent stroke.
Treatment for atrial fibrillation may include medications, therapy to reset the heart rhythm and catheter procedures to block faulty heart signals.
A person with atrial fibrillation may also have a related heart rhythm problem called atrial flutter. Although atrial flutter is a different arrhythmia, the treatment is quite similar to atrial fibrillation.
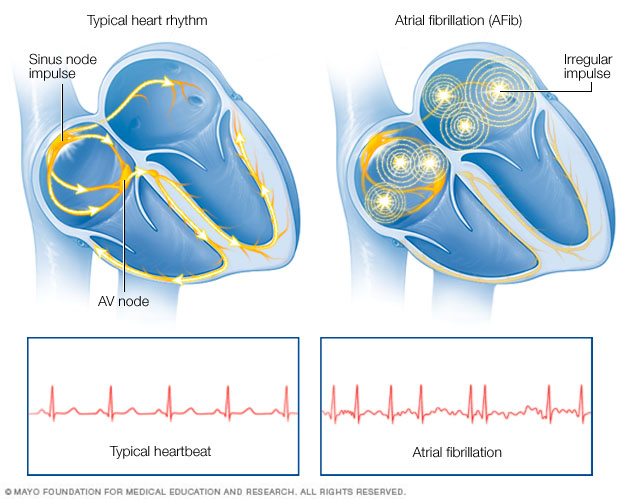
In a typical heart, a tiny cluster of cells at the sinus node sends out an electrical signal. The signal then travels through the atria to the atrioventricular (AV) node and passes into the ventricles, causing them to contract and pump out blood. In atrial fibrillation, electrical signals fire from multiple locations in the atria (typically pulmonary veins), causing them to beat chaotically. Since the atrioventricular (AV) node doesn't prevent all of these chaotic signals from entering the ventricles, the heart beats faster and irregularly.
Symptoms
Some people with atrial fibrillation (A-fib) don't notice any symptoms. Those who do have atrial fibrillation symptoms may have signs and symptoms such as:
- Sensations of a fast, fluttering or pounding heartbeat (palpitations)
- Chest pain
- Dizziness
- Fatigue
- Lightheadedness
- Reduced ability to exercise
- Shortness of breath
- Weakness
Atrial fibrillation may be:
- Occasional (paroxysmal atrial fibrillation). A-fib symptoms come and go, usually lasting for a few minutes to hours. Sometimes symptoms occur for as long as a week and episodes can happen repeatedly. Symptoms might go away on their own. Some people with occasional A-fib need treatment.
- Persistent. With this type of atrial fibrillation, the heart rhythm doesn't go back to normal on its own. If a person has A-fib symptoms, cardioversion or treatment with medications may be used to restore and maintain a normal heart rhythm.
- Long-standing persistent. This type of atrial fibrillation is continuous and lasts longer than 12 months.
- Permanent. In this type of atrial fibrillation, the irregular heart rhythm can't be restored. Medications are needed to control the heart rate and to prevent blood clots.
When to see a doctor
If you have any signs or symptoms of atrial fibrillation, make an appointment with your doctor.
If you have chest pain, seek immediate medical help. Chest pain could mean that you're having a heart attack.
Causes
To understand the causes of A-fib, it may be helpful to know how the heart typically beats.
The typical heart has four chambers — two upper chambers (atria) and two lower chambers (ventricles). Within the upper right chamber of the heart (right atrium) is a group of cells called the sinus node. The sinus node is the heart's natural pacemaker. It produces the signal that starts each heartbeat.
In a regular heart rhythm:
- The signal travels from the sinus node through the two upper heart chambers (atria).
- The signal passes through a pathway between the upper and lower chambers called the atrioventricular (AV) node.
- The movement of the signal causes your heart to squeeze (contract), sending blood to your heart and body.
In atrial fibrillation, the signals in the upper chambers of the heart are chaotic. As a result, the upper chambers shake (quiver). The AV node is then bombarded with signals trying to get through to the lower heart chambers (ventricles). This causes a fast and irregular heart rhythm.
The heart rate in atrial fibrillation may range from 100 to 175 beats a minute. The normal range for a heart rate is 60 to 100 beats a minute.
Causes of atrial fibrillation
Problems with the heart's structure are the most common cause of atrial fibrillation. Possible causes of atrial fibrillation include:
- Coronary artery disease
- Heart attack
- Heart defect that you're born with (congenital heart defect)
- Heart valve problems
- High blood pressure
- Lung diseases
- Physical stress due to surgery, pneumonia or other illnesses
- Previous heart surgery
- Problem with the heart's natural pacemaker (sick sinus syndrome)
- Sleep apnea
- Thyroid disease such as an overactive thyroid (hyperthyroidism) and other metabolic imbalances
- Use of stimulants, including certain medications, caffeine, tobacco and alcohol
- Viral infections
Some people who have atrial fibrillation have no known heart problems or heart damage.
Risk factors
Things that can increase the risk of atrial fibrillation (A-fib) include:
- Age. The older a person is, the greater the risk of developing atrial fibrillation.
- Heart disease. Anyone with heart disease — such as heart valve problems, congenital heart disease, congestive heart failure, coronary artery disease, or a history of heart attack or heart surgery — has an increased risk of atrial fibrillation.
- High blood pressure. Having high blood pressure, especially if it's not well controlled with lifestyle changes or medications, can increase the risk of atrial fibrillation.
- Thyroid disease. In some people, thyroid problems may trigger heart rhythm problems (arrhythmias), including atrial fibrillation.
- Other chronic health conditions. People with certain chronic conditions such as diabetes, metabolic syndrome, chronic kidney disease, lung disease or sleep apnea have an increased risk of atrial fibrillation.
- Drinking alcohol. For some people, drinking alcohol can trigger an episode of atrial fibrillation. Binge drinking further increases the risk.
- Obesity. People who have obesity are at higher risk of developing atrial fibrillation.
- Family history. An increased risk of atrial fibrillation occurs in some families.
Complications
Blood clots are a dangerous complication of atrial fibrillation that can lead to stroke.
In atrial fibrillation, the chaotic heart rhythm can cause blood to collect in the heart's upper chambers (atria) and form clots. If a blood clot in the left upper chamber (left atrium) breaks free from the heart area, it can travel to the brain and cause a stroke.
The risk of stroke from atrial fibrillation increases as you grow older. Other health conditions also may increase your risk of a stroke due to A-fib, including:
- High blood pressure
- Diabetes
- Heart failure
- Some valvular heart disease
Blood thinners are commonly prescribed to prevent blood clots and strokes in people with atrial fibrillation.
Prevention
Healthy lifestyle choices can reduce the risk of heart disease and may prevent atrial fibrillation. Here are some basic heart-healthy tips:
- Eat a nutritious diet
- Get regular exercise and maintain a healthy weight
- Don't smoke
- Avoid or limit alcohol and caffeine
- Manage stress, as intense stress and anger can cause heart rhythm problems
Diagnosis
Some people are unaware that they have atrial fibrillation (A-fib). A-fib may be detected when a doctor is listening to the heart with a stethoscope during a physical exam for other reasons.
A doctor may order several tests to diagnose A-fib or exclude other conditions that can cause similar symptoms. Tests may include:
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. Sticky patches (electrodes) are placed on the chest and sometimes the arms and legs. Wires connect the electrodes to a computer, which displays the test results. An ECG can show if the heart is beating too fast, too slow or not at all. An ECG is the main test for diagnosing atrial fibrillation.
- Blood tests. These help a doctor rule out thyroid problems or detect other substances in the blood that may lead to A-fib.
- Holter monitor. This small, portable ECG device is carried in a pocket or worn on a belt or shoulder strap during regular daily activities. It records the heart's activity continuously for 24 hours or longer.
- Event recorder. This device is similar to a Holter monitor, but it records only at certain times for a few minutes at a time. It's worn longer than a Holter monitor, typically 30 days. You generally push a button when you feel symptoms. Some devices automatically record when an irregular heart rhythm is detected.
- Echocardiogram. This noninvasive test uses sound waves to create images of the heart's size, structure and motion.
- Stress test. Also called exercise testing, stress testing involves running tests on the heart while exercising on a treadmill or stationary bike.
- Chest X-ray. X-ray images help a doctor see the condition of the lungs and heart.
Treatment
Treatment for atrial fibrillation depends on how long you've had A-fib, your symptoms and the underlying cause of the heartbeat problem. The goals of treatment are to:
- Reset the heart rhythm
- Control the heart rate
- Prevent blood clots that can lead to stroke
Atrial fibrillation treatment may involve:
- Medications
- Therapy to reset the heart rhythm (cardioversion)
- Surgery or catheter procedures
Together, you and your doctors will discuss the best treatment option for you. It's important to follow your atrial fibrillation treatment plan. If A-fib isn't well controlled, it may lead to other complications, including strokes and heart failure.
Medications
You may be prescribed medications to control how fast your heart beats and restore it to a normal rate. Medications are also prescribed to prevent blood clots, a dangerous complication of A-fib.
Medications used to treat atrial fibrillation include:
- Beta blockers. These medications can help slow the heart rate at rest and during activity.
- Calcium channel blockers. These medicines control the heart rate but may need to be avoided by those who have heart failure or low blood pressure.
- Digoxin. This medication may control the heart rate at rest, but not as well during activity. Most people need additional or alternative medications, such as calcium channel blockers or beta blockers.
- Anti-arrhythmic medications. These drugs are used to maintain a normal heart rhythm, not just to control the heart rate. Because they tend to have more side effects than drugs that control the heart rate, anti-arrhythmics tend to be used more sparingly.
- Blood thinners. To reduce the risk of stroke or damage to other organs caused by blood clots, a doctor may prescribe a blood-thinning medication (anticoagulant). Blood thinners include warfarin (Jantoven), apixaban (Eliquis), dabigatran (Pradaxa), edoxaban (Savaysa) and rivaroxaban (Xarelto). If you take warfarin, you'll need to have regular blood tests to monitor the drug's effects.
Cardioversion therapy
If A-fib symptoms are bothersome or if this is the first episode of atrial fibrillation, a doctor may attempt to reset the heart rhythm (sinus rhythm) using a procedure called cardioversion.
Cardioversion can be done in two ways:
- Electrical cardioversion. This method to reset the heart rhythm is done by sending electric shocks to the heart through paddles or patches (electrodes) placed on the chest.
- Drug cardioversion. Medications given through an IV or by mouth are used to reset the heart rhythm.
Cardioversion is usually done in a hospital as a scheduled procedure, but it may be done in emergency situations. If it's scheduled, warfarin (Jantoven) or another blood thinner may be given a few weeks before it's done to reduce the risk of blood clots and strokes.
After electrical cardioversion, anti-arrhythmic medications may be prescribed indefinitely to help prevent future episodes of atrial fibrillation. Even with medications, there is a chance of another episode of atrial fibrillation.
Surgery or catheter procedures
If A-fib doesn't get better with medications or other therapies, a doctor might recommend a procedure called cardiac ablation. Sometimes ablation is the first treatment for certain patients.
Cardiac ablation uses heat (radiofrequency energy) or extreme cold (cryoablation) to create scars in your heart to block abnormal electrical signals and restore a normal heartbeat. A doctor inserts a flexible tube (catheter) through a blood vessel, usually in your groin, and into your heart. More than one catheter may be used. Sensors on the tip of the catheter apply the cold or heat energy.
Less commonly, ablation is performed using a scalpel during open-heart surgery.
There are different types of cardiac ablation. The type used to treat atrial fibrillation depends on your specific symptoms, overall health and whether you're having another heart surgery.
For example, some of the types of cardiac ablation that may be used to treat atrial fibrillation are:
- Atrioventricular (AV) node ablation. Heat or cold energy is applied to the heart tissue at the AV node to destroy the electrical signaling connection. After AV node ablation, a pacemaker is needed for life.
-
Maze procedure. A doctor uses heat or cold energy or a scalpel to create a pattern of scar tissue (the maze) in the upper chambers of the heart. Because scar tissue doesn't send electrical signals, the maze interferes with the stray heart signals that cause atrial fibrillation.
If a scalpel is used to create the maze pattern, open-heart surgery is necessary. This is called the surgical maze procedure. It's the preferred method of atrial fibrillation treatment in those who need another heart surgery, such as coronary artery bypass surgery or heart valve repair.
Atrial fibrillation may return after cardiac ablation. If this happens, another cardiac ablation or other heart treatment may be recommended. After cardiac ablation, lifelong blood thinners may be needed to prevent strokes.
If a person with A-fib can't take blood-thinning medications, a doctor may recommend a catheter procedure to seal a small sac (appendage) in the left upper heart chamber, where most A-fib related clots form. This procedure is called left atrial appendage closure. A closure device is gently guided through a catheter to the sac. Once the device is in place, the catheter is removed. The device is left permanently in place. Surgery to close the left atrial appendage is an option for some people already having heart surgery.
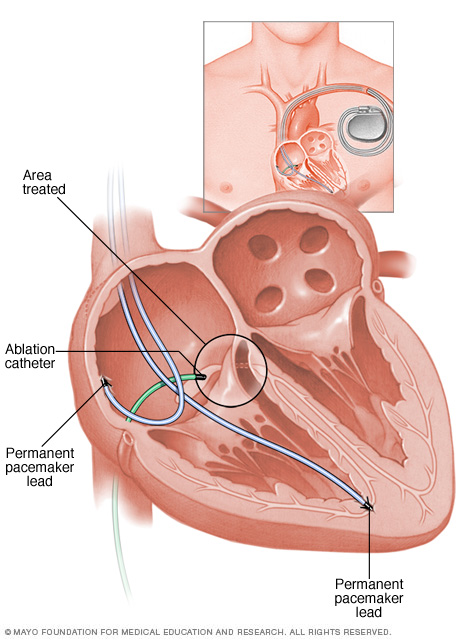
In atrioventricular (AV) node ablation, a heart doctor uses radiofrequency energy to destroy the electrical connection between the upper and lower heart chambers (AV node), blocking the heart's electrical impulses. Once the AV node is destroyed, the heart doctor then implants a small medical device to maintain a heart rhythm (pacemaker).
Lifestyle and home remedies
Following a heart-healthy lifestyle can help prevent or treat conditions such as high blood pressure and heart disease. Lifestyle changes often include:
- Eating heart-healthy foods. Eat a healthy diet that's low in salt and solid fats and rich in fruits, vegetables and whole grains.
- Exercising regularly. Exercise daily and increase physical activity.
- Quitting smoking. If you smoke and can't quit on your own, talk to your doctor about strategies or programs to help you break a smoking habit.
- Maintaining a healthy weight. Being overweight increases your risk of developing heart disease. Healthy weight loss can help to manage symptoms of atrial fibrillation and may improve the results of catheter ablation.
- Keeping blood pressure and cholesterol levels under control. Make lifestyle changes and take medications as prescribed to correct high blood pressure (hypertension) or high cholesterol.
- Limiting alcohol. Binge drinking (having five drinks in two hours for men or four drinks for women) can increase the chances of atrial fibrillation. In some people, even modest amounts of alcohol can trigger atrial fibrillation.
- Getting follow-up care. Take your medications as prescribed and have regular follow-up appointments with your doctor. Tell your doctor if your symptoms worsen.
Preparing for an appointment
If you have an irregular or pounding heartbeat, make an appointment with your family doctor. If atrial fibrillation is found early, treatment may be easier and more effective. You may be referred to a doctor trained in heart conditions (cardiologist).
Because appointments can be brief, and because there's often a lot to discuss, it's a good idea to be prepared for your appointment. Here's some information to help you get ready for your appointment, and what to expect from your doctor.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your dietary intake. You may need to do this if your doctor orders blood tests.
- Write down any symptoms you're experiencing, including any that may seem unrelated to atrial fibrillation.
- Write down key personal information, including any family history of heart disease, stroke, high blood pressure or diabetes, and any major stresses or recent life changes.
- Make a list of all medications, vitamins or supplements that you're taking.
- Take a family member or friend along, if possible. Sometimes it can be difficult to understand and remember all the information provided to you during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your doctor.
Your time with your doctor is limited, so preparing a list of questions will help you make the most of your time together. List your questions from most important to least important, in case time runs out. For atrial fibrillation, some basic questions to ask your doctor include:
- What is likely causing my symptoms or condition?
- What are other possible causes for my symptoms or condition?
- What kinds of tests will I need?
- What's the most appropriate treatment?
- What foods should I eat or avoid?
- What's an appropriate level of physical activity?
- How often should I be screened for heart disease or other complications of atrial fibrillation?
- What are the alternatives to the primary approach that you're suggesting?
- I have other health conditions. How can I best manage them together?
- Are there any restrictions that I need to follow?
- Should I see a specialist? What will that cost, and will my insurance cover seeing a specialist? (You may need to ask your insurance provider directly for information about coverage.)
- Is there a generic alternative to the medicine you're prescribing?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
In addition to the questions that you've prepared to ask your doctor, don't hesitate to ask questions during your appointment.
What to expect from your doctor
Your doctor is likely to ask you a number of questions. Being ready to answer them may save time to go over any points you want to spend more time on. Your doctor may ask:
- When did you first begin experiencing symptoms?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Copyright © 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.