Endocarditis is a life-threatening inflammation of the inner lining of the heart's chambers and valves. This lining is called the endocardium.
Endocarditis is usually caused by an infection. Bacteria, fungi or other germs get into the bloodstream and attach to damaged areas in the heart. Things that make you more likely to get endocarditis are artificial heart valves, damaged heart valves or other heart defects.
Without quick treatment, endocarditis can damage or destroy the heart valves. Treatments for endocarditis include medications and surgery.
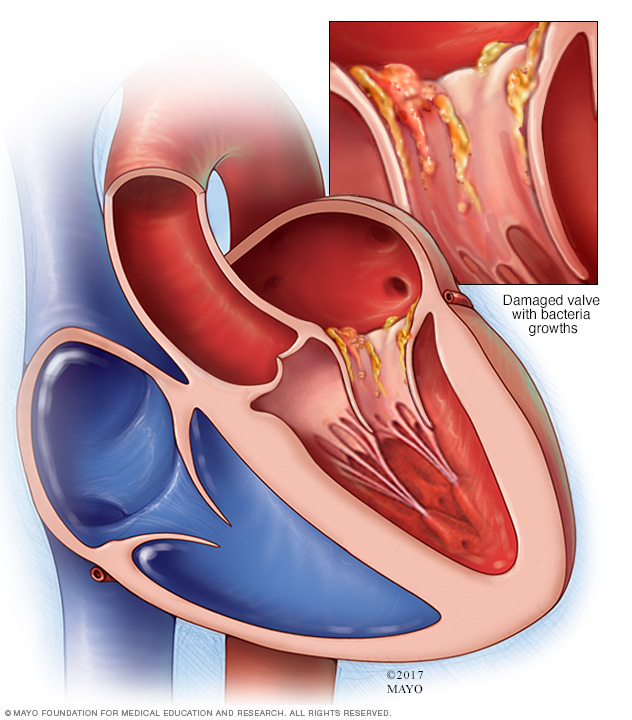
Endocarditis occurs when bacteria or other germs enter the bloodstream and travel to the heart. The germs then stick to damaged heart valves or damaged heart tissue.
Symptoms
Symptoms of endocarditis can vary from person to person. Endocarditis may develop slowly or suddenly. It depends on the type of germs causing the infection and whether there are other heart problems.
Common symptoms of endocarditis include:
- Aching joints and muscles
- Chest pain when you breathe
- Fatigue
- Flu-like symptoms, such as fever and chills
- Night sweats
- Shortness of breath
- Swelling in the feet, legs or belly
- A new or changed whooshing sound in the heart (murmur)
Less common endocarditis symptoms can include:
- Unexplained weight loss
- Blood in the urine
- Tenderness under the left rib cage (spleen)
- Painless red, purple or brown flat spots on the soles bottom of the feet or the palms of the hands (Janeway lesions)
- Painful red or purple bumps or patches of darkened skin (hyperpigmented) on the tips of the fingers or toes (Osler nodes)
- Tiny purple, red or brown round spots on the skin (petechiae), in the whites of the eyes or inside the mouth
When to see a doctor
If you have symptoms of endocarditis, see your health care provider as soon as possible — especially if you have a congenital heart defect or history of endocarditis. Less serious conditions may cause similar signs and symptoms. A proper evaluation by a health care provider is needed to make the diagnosis.
If you've been diagnosed with endocarditis and have any of the following symptoms, tell your care provider. These symptoms may mean the infection is getting worse:
- Chills
- Fever
- Headaches
- Joint pain
- Shortness of breath
Causes
Endocarditis is usually caused by an infection with bacteria, fungi or other germs. The germs enter the bloodstream and travel to the heart. In the heart, they attach to damaged heart valves or damaged heart tissue.
Usually, the body's immune system destroys any harmful bacteria that enter the bloodstream. However, bacteria on the skin or in the mouth, throat or gut (intestines) may enter the bloodstream and cause endocarditis under the right circumstances.
Risk factors
Many different things can cause germs to get into the bloodstream and lead to endocarditis. Having a faulty, diseased or damaged heart valve increases the risk of the condition. However, endocarditis may occur in those without heart valve problems.
Risk factors for endocarditis include:
- Older age. Endocarditis occurs most often in adults over age 60.
- Artificial heart valves. Germs are more likely to attach to an artificial (prosthetic) heart valve than to a regular heart valve.
- Damaged heart valves. Certain medical conditions, such as rheumatic fever or infection, can damage or scar one or more of the heart valves, increasing the risk of infection. A history of endocarditis also increases the risk of infection.
- Congenital heart defects. Being born with certain types of heart defects, such as an irregular heart or damaged heart valves, raises the risk of heart infections.
- Implanted heart device. Bacteria can attach to an implanted device, such as a pacemaker, causing an infection of the heart's lining.
- Illegal IV drug use. Using dirty IV needles can lead to infections such as endocarditis. Contaminated needles and syringes are a special concern for people who use illegal IV drugs, such as heroin or cocaine.
- Poor dental health. A healthy mouth and healthy gums are essential for good health. If you don't brush and floss regularly, bacteria can grow inside your mouth and may enter your bloodstream through a cut on your gums. Some dental procedures that can cut the gums also may allow bacteria to get in the bloodstream.
- Long-term catheter use. A catheter is a thin tube that's used to do some medical procedures. Having a catheter in place for a long period of time (indwelling catheter) increases the risk of endocarditis.
If you're at risk of endocarditis, tell your health care providers. You may want to request an endocarditis wallet card from the American Heart Association. Check with your local chapter or print the card from the association's website.
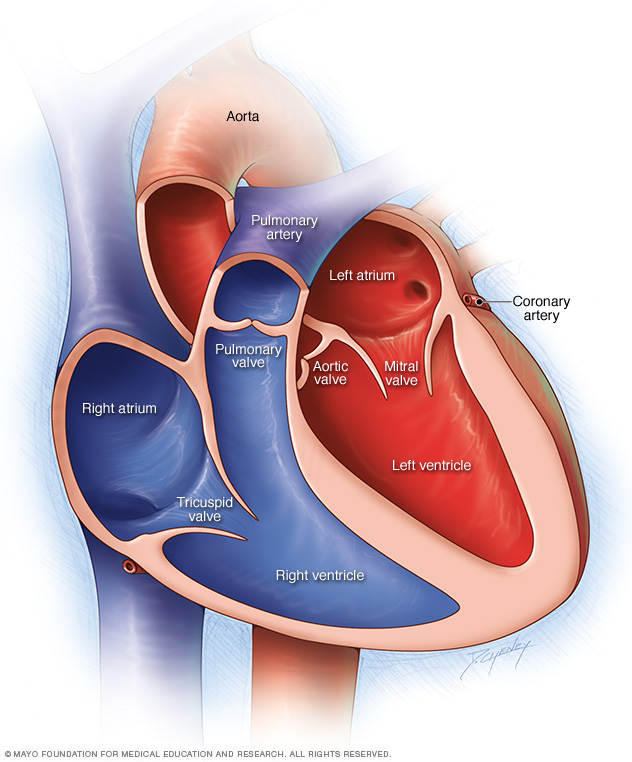
A typical heart has two upper and two lower chambers. The upper chambers — the right and left atria — receive incoming blood. The lower chambers — the right and left ventricles — pump blood out of your heart. The heart valves, which keep blood flowing in the right direction, are gates at the chamber openings (for the tricuspid and mitral valves) and exits (for the pulmonary and aortic valves).
Complications
In endocarditis, irregular growths made of germs and cell pieces form a mass in the heart. These clumps are called vegetations. They can break loose and travel to the brain, lungs, kidneys and other organs. They can also travel to the arms and legs.
Complications of endocarditis may include:
- Heart failure
- Heart valve damage
- Stroke
- Pockets of collected pus (abscesses) that develop in the heart, brain, lungs and other organs
- Blood clot in a lung artery (pulmonary embolism)
- Kidney damage
- Enlarged spleen
Prevention
You can take the following steps to help prevent endocarditis:
- Know the signs and symptoms of endocarditis. See your health care provider immediately if you develop any symptoms of infection — especially a fever that won't go away, unexplained fatigue, any type of skin infection, or open cuts or sores that don't heal properly.
- Take care of your teeth and gums. Brush and floss your teeth and gums often. Get regular dental checkups. Good dental hygiene is an important part of maintaining your overall health.
- Don't use illegal IV drugs. Dirty needles can send bacteria into the bloodstream, increasing the risk of endocarditis.
Preventive antibiotics
Certain dental and medical procedures may allow bacteria to enter your bloodstream.
If you're at high risk of endocarditis, the American Heart Association recommends taking antibiotics an hour before having any dental work done.
You're at high risk of endocarditis and need antibiotics before dental work if you have:
- A history of endocarditis
- A mechanical heart valve
- A heart transplant, in some cases
- Certain types of congenital heart disease
- Congenital heart disease surgery in the last six months
If you have endocarditis or any type of congenital heart disease, talk to your dentist and other care providers about your risks and whether you need preventive antibiotics.
Diagnosis
To diagnose endocarditis, a health care provider does a physical exam and asks questions about your medical history and symptoms. Tests are done to help confirm or rule out endocarditis.
Tests
Tests used to help diagnose endocarditis include:
- Blood culture test. This test helps identify germs in the bloodstream. Results from this test help determine the antibiotic or combination of antibiotics to use for treatment.
- Complete blood count. This test can determine if there's a lot of white blood cells, which can be a sign of infection. A complete blood count can also help diagnose low levels of healthy red blood cells (anemia), which can be a sign of endocarditis. Other blood tests also may be done.
-
Echocardiogram. Sound waves are used to create images of the beating heart. This test shows how well the heart's chambers and valves pump blood. It can also show the heart's structure. Your provider may use two different types of echocardiograms to help diagnose endocarditis.
In a standard (transthoracic) echocardiogram, a wandlike device (transducer) is moved over the chest area. The device directs sound waves at the heart and records them as they bounce back.
In a transesophageal echocardiogram, a flexible tube containing a transducer is guided down the throat and into the tube connecting the mouth to the stomach (esophagus). A transesophageal echocardiogram provides much more detailed pictures of the heart than is possible with a standard echocardiogram.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. During an ECG, sensors (electrodes) are attached to the chest and sometimes to the arms or legs. It isn't specifically used to diagnose endocarditis, but it can show if something is affecting the heart's electrical activity.
- Chest X-ray. A chest X-ray shows the condition of the lungs and heart. It can help determine if endocarditis has caused heart swelling or if any infection has spread to the lungs.
- Computerized tomography (CT) scan or magnetic resonance imaging (MRI). You may need scans of your brain, chest or other parts of your body if your provider thinks that infection has spread to these areas.
Treatment
Many people with endocarditis are successfully treated with antibiotics. Sometimes, surgery may be needed to fix or replace damaged heart valves and clean up any remaining signs of the infection.
Medications
The type of medication you receive depends on what's causing the endocarditis.
High doses of IV antibiotics are used to treat endocarditis caused by bacteria. If you receive IV antibiotics, you'll generally spend a week or more in the hospital so that care providers can determine if the treatment is working.
Once your fever and any severe symptoms have gone away, you might be able to leave the hospital. Some people continue IV antibiotics with visits to a provider's office or at home with home care. Antibiotics are usually taken for several weeks.
If endocarditis is caused by a fungal infection, antifungal medication is given. Some people need lifelong antifungal pills to prevent endocarditis from returning.
Surgery or other procedures
Heart valve surgery may be needed to treat persistent endocarditis infections or to replace a damaged valve. Surgery is sometimes needed to treat endocarditis that's caused by a fungal infection.
Depending on your specific condition, your health care provider may recommend heart valve repair or replacement. Heart valve replacement uses a mechanical valve or a valve made from cow, pig or human heart tissue (biologic tissue valve).
Preparing for an appointment
The first health care provider you see will likely be your primary care provider or an emergency room doctor. You may be referred to a doctor or surgeon trained in diagnosing and treating heart conditions (cardiologist).
What you can do
You can help prepare for your appointment by taking these steps:
- Write down any symptoms you're having. Be sure to note how long you've had them. If you've had similar symptoms that have come and gone in the past, be sure to include that information.
- Make a list of important medical information. Write down any other recent health problems you've had. List the names of all medicines and supplements you're taking. Include their dosages.
- Ask a family member or friend to come with you to the appointment. Someone who goes with you can help remember what your provider says.
It's also important to write down any questions you might have before you get to your appointment. For endocarditis, some basic questions you might want to ask your health care provider include:
- What's the most likely cause of my symptoms?
- What kinds of tests do I need? How do I need to prepare for the tests?
- What treatment do you recommend?
- How soon after I begin treatment will I start to feel better?
- What are the possible side effects?
- Am I at risk of long-term complications from this condition? Will it come back?
- How often will I need follow-up for this condition?
- Do I need to take preventive antibiotics for certain medical or dental procedures?
- I have other medical conditions. How can I best manage these conditions together?
What to expect from your doctor
Your health care provider will probably ask you many questions, including:
- What are your symptoms?
- When did your symptoms start? Did they come on suddenly or more gradually?
- Have you had similar symptoms in the past?
- Are you having difficulty breathing?
- Have you recently had an infection?
- Have you recently had a fever?
- Have you recently had any medical or dental procedures that used needles or catheters?
- Have you ever used IV drugs?
- Have you recently lost weight without trying?
- Have you been diagnosed with any other medical conditions, especially heart murmurs?
- Do any of your first-degree relatives — such as parents, siblings or children — have a history of heart disease?
Copyright © 1998-2025 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.